Your Benefit Payment
Payment Schedule
The 2026 pension payment schedule is available below. View the full schedule for detailed monthly payment dates.
Paystub Codes Defined
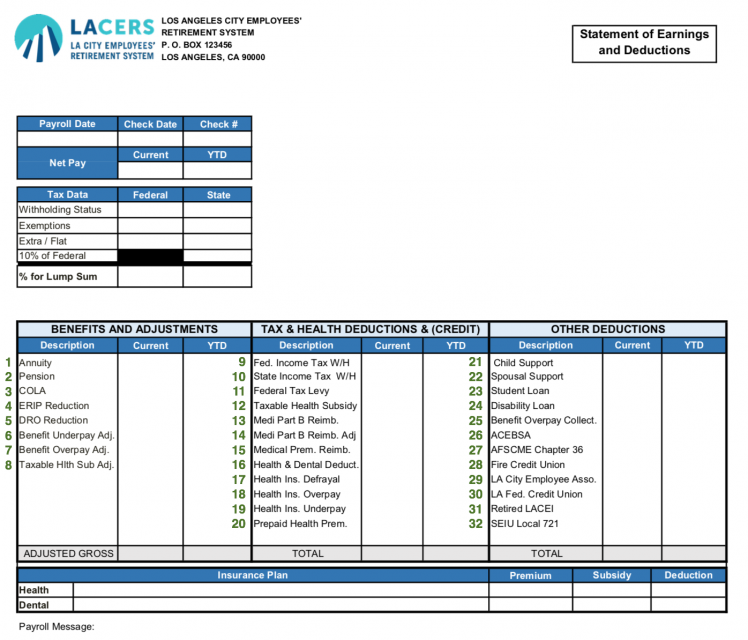
In order to help you better understand the different codes on your LACERS retirement benefit paystubs, we have provided the following explanation of terms for your reference:
*Please refer to the sample paystub shown here, which contains numbered entries that correspond to the terms listed below.
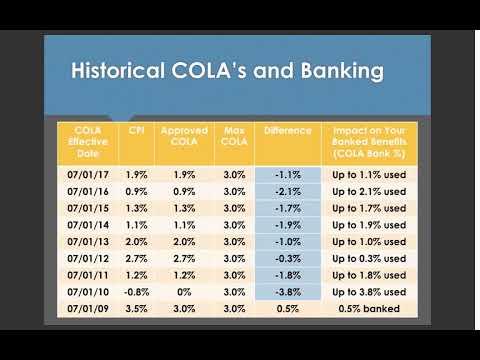
Cost of Living Adjustments (COLA)
Each year the LACERS Board approves Cost-of-Living Adjustments (COLAs)for Tier 1 and Tier 3 Retired Members and beneficiaries based on the Consumer Price Index (CPI) for the Los Angeles area during the previous calendar year. The COLA becomes effective July 1st of each year.
Benefit Verification Requests
You may request a benefit verification letter (also known as an “Award Letter”) via your MyLACERS account or by submitting the Verification of Pension Request form to our office by secure document upload, fax, or mail.
1099-R Tax Form
LACERS 1099-R MAILINGS
LACERS mails 1099-R tax documents to retirees and beneficiaries for the previous tax year on or before January 31 in accordance with Internal Revenue Service (IRS) rules. 1099-Rs can also be viewed and printed inside MyLACERS accounts. Please note that 1099-Rs are only sent to the address on file with LACERS.